A new MIT study finds that Alzheimer’s disease disrupts at least one form of visual memory by degrading a newly identified circuit that connects the vision processing centers of each brain hemisphere.
The results of the study, published in Neuron by a research team based at The Picower Institute for Learning and Memory, come from experiments in mice, but provide a physiological and mechanistic basis for prior observations in human patients: the degree of diminished brain rhythm synchrony between counterpart regions in each hemisphere correlates with the clinical severity of dementia.
“We demonstrate that there is a functional circuit that can explain this phenomenon,” says lead author Chinnakkaruppan Adaikkan, a former Picower Institute postdoc who is now an assistant professor in the Centre for Brain Research at the Indian Institute of Science (IISc) in Bangalore. “In a way, we uncovered a fundamental biology that was not known before.”
Specifically, Adaikkan’s work identified neurons that connect the primary visual cortex (V1) of each hemisphere and showed that when the cells are disrupted, either by genetic alterations that model Alzheimer’s disease or by direct laboratory perturbations, brain rhythm synchrony becomes reduced and mice become significantly less able to notice when a new pattern appeared on a wall in their enclosures. Such recognition of novelty, which requires visual memory of what was there the prior day, is an ability commonly disrupted in Alzheimer’s.
“This study demonstrates the propagation of gamma rhythm synchrony across the brain hemispheres via the cross hemispheric connectivity,” says study senior author Li-Huei Tsai, Picower Professor and director of The Picower Institute and MIT’s Aging Brain Initiative. “It also demonstrates that the disruption of this circuit in AD mouse models is associated with specific behavioral deficits.”
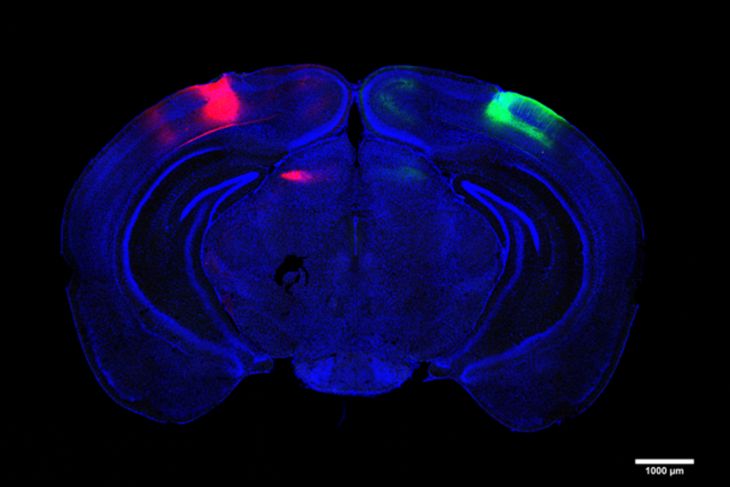
In the study, Adaikkan, Tsai, Thomas McHugh, and co-authors discovered and traced V1 neurons that extended their axons all the way through the corpus callosum, which connects the brain’s hemispheres, to cells in the V1 on the brain’s other side. There, they found, the cross-hemispheric (CH) neurons forged connections, or synapses, with target cells, providing them with “excitatory” stimulation to drive their activity. Adaikkan also found that CH neurons were much more likely to be activated by a novelty discrimination task than V1 neurons in general or neurons in other regions heavily involved in memory such as the hippocampus or the prefrontal cortex.
Curious about how this might differ in Alzheimer’s disease, the team looked at the activity of the cells in two different Alzheimer’s mouse models. The found that CH cell activity was significantly lessened amid the disease. Unsurprisingly, Alzheimer’s mice fared much poorer in novelty discrimination tasks.
The team examined the CH cells closely and found that they gather incoming input from a variety of other cells within their V1 and other regions in their hemisphere that process visual information. When they compared the incoming connections of healthy CH neurons to those in CH cells afflicted with Alzheimer’s, they found that cells in the disease condition had significantly less infrastructure for hosting incoming connections (measured in terms of synapse-hosting spines protruding from the vine-like dendrites that sprawl out of the cell body).
Given the observations correlating reduced brain rhythm synchrony and memory performance in Alzheimer’s, the team wondered if that occurred in the mice, too. To find out, they custom-designed electrodes to measure rhythmic activity simultaneously in all cortical layers of each hemisphere’s V1. They observed that cross-hemispheric synchrony increased notably between the V1s when mice engaged in novelty discrimination but that the synchrony, both at high “gamma” and lower “theta” frequency rhythms, was significantly lower in the Alzheimer’s mice than it was in healthy mice.
Adaikkan’s evidence at that point was strong, but still only suggestive, that CH neurons provided the means by which the V1 regions on each side of the brain could coordinate to enable novelty discrimination, and that this ability became undermined by Alzheimer’s degradation of the CH cells’ connectivity. To more directly determine whether the CH circuit played such a causal, consequential role, the team directly intervened to disrupt them, testing what effect targeted perturbations had.
They found that chemically inhibiting CH cells disrupted rhythm synchrony between V1s, mirroring measures made in Alzheimer’s model mice. Moreover, disrupting CH activity undermined novelty discrimination ability. To further test whether it was the cells’ cross-hemispheric nature that mattered specifically, they engineered CH cells to be controllable with flashes of light (a technology called “optogenetics”). When they shined the light on the connections, they forged in the other hemisphere to inhibit those, they found that doing so again compromised visual discrimination ability.
All together, the study results show that CH cells in V1 connect with neurons in the counterpart area of the opposite hemisphere to synchronize neural activity needed for properly recognizing novelty, but that Alzheimer’s disease damages their ability to do that job.
Adaikkan says he is curious to now look at other potential cross-hemispheric connections and how they may be affected in Alzheimer’s disease, too. He says he also wants to study what happens to synchrony at other rhythm frequencies.
In addition to Adaikkan, Tsai, and McHugh, the study’s other authors are Jun Wang, Karim Abdelall, Steven Middleton, Lorenzo Bozzelli, and Ian Wickersham.
The JPB Foundation, The National Institutes of Health, and the Robert A. and Renee E. Belfer Foundation provided funding for the study.